What Is Happening at the Injection Site
Injection site reactions (ISRs) are the most common side effect of subcutaneous peptide use, affecting approximately 5-30% of users depending on the peptide. The typical presentation: redness (erythema), swelling, itching, warmth, and sometimes a small firm lump (induration) at or near the injection site. These reactions usually appear within 30 minutes to 4 hours after injection and resolve within 24-72 hours.
The biological mechanism varies by cause: (1) Histamine release — many peptides (especially GHRPs like GHRP-2, GHRP-6, and to a lesser extent ipamorelin) stimulate mast cell degranulation at the injection site, releasing histamine. Histamine causes vasodilation (redness), increased vascular permeability (swelling), and nerve fiber stimulation (itching). This is a pharmacological effect, not a contamination issue. (2) Foreign body response — the immune system may recognize the peptide or excipients as foreign, triggering a localized inflammatory response with neutrophil and macrophage infiltration. (3) Tissue irritation — residual solvents (particularly TFA), acidic or basic pH of the reconstituted solution, or high concentration can irritate subcutaneous tissue directly.
Most ISRs are mild and self-limiting. They are annoying but not dangerous. However, distinguishing between a normal histamine reaction and an infection or allergic response is important for safety.
Prevention Strategies That Actually Work
Based on clinical evidence and community experience, the following strategies reduce ISR frequency and severity: (1) Rotate injection sites systematically — use an alternating pattern across at least 4-6 sites (left and right lower abdomen, left and right upper thigh, left and right upper arm/deltoid). Do not inject the same site twice within 7 days. Rotation prevents localized tissue inflammation accumulation.
(2) Allow the alcohol swab to dry completely before injecting — injecting through wet alcohol pushes the alcohol into subcutaneous tissue, causing a burning sensation and chemical irritation. Wait 15-30 seconds after swabbing. (3) Inject slowly — rapid injection creates tissue trauma and pressure. A 250 mcg peptide dose in a typical volume (0.05-0.2 mL) should be injected over 5-10 seconds, not as a quick push.
(4) Ensure reconstituted solution is at room temperature — cold solution from the refrigerator can cause vasoconstriction and irritation. Remove the vial from the refrigerator 10-15 minutes before injection. (5) Consider antihistamine pre-treatment if histamine-mediated reactions are frequent — loratadine (Claritin) 10 mg or cetirizine (Zyrtec) 10 mg taken 30-60 minutes before injection can significantly reduce histamine-related ISRs. (6) Use proper needle gauge — 27-31 gauge needles are standard for subcutaneous peptide injection. Larger gauges cause more tissue trauma.
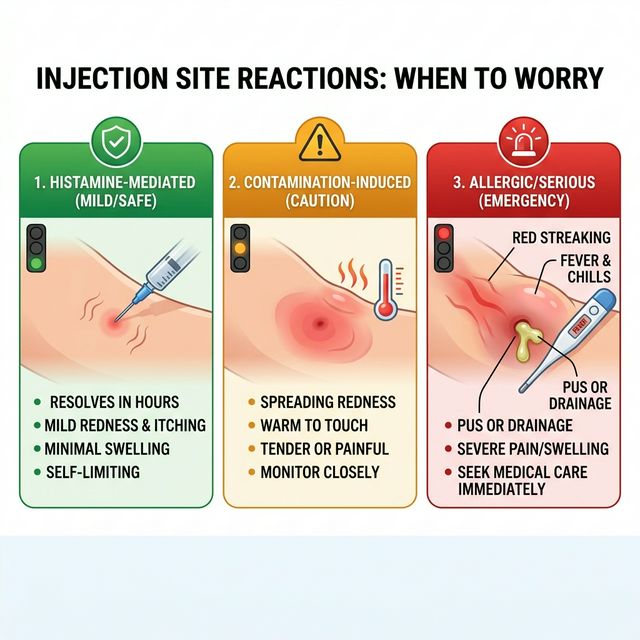
When to Be Concerned: Red Flags
Seek medical attention if you experience: (1) Spreading redness that expands beyond 5 cm from the injection site, especially with warmth and pain — this may indicate cellulitis (bacterial skin infection) requiring antibiotics. (2) Red streaking extending from the injection site toward nearby lymph nodes — this suggests lymphangitis and requires urgent medical evaluation. (3) Fever (temperature above 38°C/100.4°F) within 24-48 hours of injection — this could indicate systemic infection, especially if accompanied by chills, malaise, or injection site purulence.
(4) Purulent drainage (pus) from the injection site — this indicates abscess formation requiring medical drainage and antibiotics. (5) Persistent swelling lasting more than 7 days — this could indicate granuloma formation, foreign body reaction, or local tissue necrosis. (6) Anaphylactic symptoms: difficulty breathing, facial/throat swelling, rapid heartbeat, dizziness, or widespread urticaria within minutes of injection — this is a medical emergency requiring immediate epinephrine and emergency services.
The vast majority of ISRs are category 1 (mild, self-limiting) and do not require medical intervention. But contaminated peptides can cause real infections, and allergic reactions — while rare — can be serious. If in doubt, err on the side of medical evaluation.