The $7 Billion Collagen Supplement Question
Oral collagen supplements are a $7 billion global industry backed by enthusiastic marketing and genuinely positive clinical data — but also by a fundamental pharmacological question that most consumers never consider: what happens to a collagen peptide after you swallow it?
Collagen is a protein made of three intertwined polypeptide chains, each approximately 1,000 amino acids long. Type I collagen (the most abundant in skin) has a molecular weight of approximately 300,000 daltons. The intestinal epithelium absorbs molecules up to approximately 600-1,000 daltons efficiently. So intact collagen cannot be absorbed orally — it must be broken down first.
Hydrolyzed collagen supplements (collagen peptides) are pre-digested: enzymatic hydrolysis breaks collagen into di- and tripeptides of 300-6,000 daltons. The smaller fragments (particularly proline-hydroxyproline and glycine-proline-hydroxyproline tripeptides) can be absorbed through intestinal peptide transporters (PepT1) and reach systemic circulation. Studies using isotope-labeled collagen confirm that hydroxyproline-containing peptides appear in blood within 1-2 hours of oral ingestion.
Do Oral Collagen Supplements Actually Work?
The clinical evidence is surprisingly positive, if modest. A meta-analysis by de Miranda et al. (Int J Dermatol, 2021) pooling 19 RCTs with 1,125 participants found that oral collagen supplementation (2.5-10 g/day for 8-24 weeks) significantly improved skin hydration, elasticity, and wrinkle depth versus placebo. The proposed mechanism: absorbed collagen di/tripeptides act not as direct building blocks (they are too scarce) but as signaling molecules that stimulate fibroblast activity — essentially tricking fibroblasts into producing more collagen by detecting collagen breakdown products in the blood.
The effect size is meaningful but not dramatic: approximately 7-15% improvement in skin hydration and 10-20% improvement in wrinkle depth over 12-24 weeks. These are measurable, statistically significant improvements — but they are not transformative for someone seeking major anti-aging results. And the evidence for joint, tendon, and hair effects is weaker than for skin.
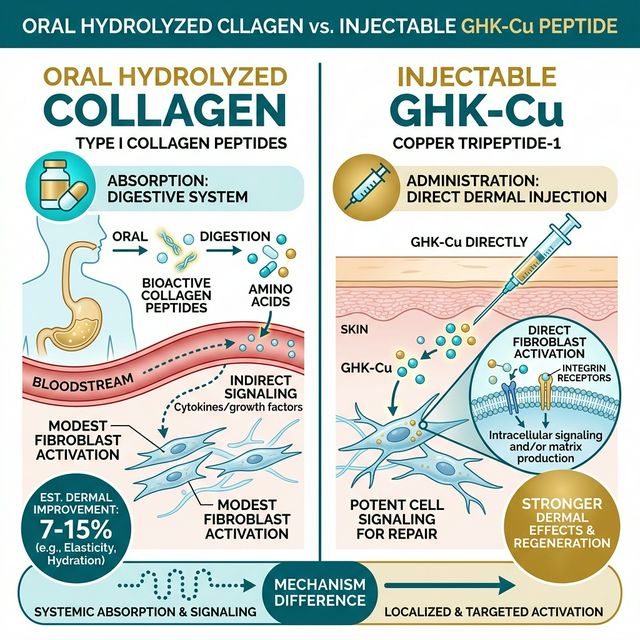
Injectable Peptides: GHK-Cu and Direct Fibroblast Stimulation
Injectable peptides like GHK-Cu take a fundamentally different approach. Instead of providing collagen fragments as indirect signals, GHK-Cu directly activates fibroblasts through copper-dependent gene regulation. GHK-Cu upregulates expression of collagen type I and III genes, elastin, decorin, glycosaminoglycans, and multiple growth factors simultaneously. The signal pathway is direct: GHK-Cu binds integrin receptors on fibroblasts, activating TGF-β signaling that stimulates extracellular matrix production.
The gene expression data is striking: Pickart et al. (2015) demonstrated that GHK-Cu treatment upregulated 31 human genes associated with extracellular matrix regeneration, while simultaneously downregulating 36 genes associated with tissue remodeling and fibrosis. The net effect is pro-regenerative collagen synthesis — new collagen deposition without scarring.
The practical difference: oral collagen supplements provide a gentle, indirect, systemic signal to fibroblasts throughout the body. Injectable GHK-Cu provides a potent, direct, targeted activation of fibroblasts at the injection site and systemically. For anti-aging skin results, the injectable approach delivers a stronger signal — but requires subcutaneous injection rather than simply drinking a powder.
Which Approach Should You Choose?
Both — they are complementary. Oral collagen supplements (10 g/day of hydrolyzed collagen) provide baseline support for skin hydration, nail and hair growth, and joint comfort with minimal cost ($20-40/month) and zero complexity. It is a reasonable foundation for anyone interested in skin health.
Injectable GHK-Cu (200-600 mcg subcutaneously daily for 30-60 day cycles) provides a more potent fibroblast activation signal for people seeking measurable anti-aging skin results — improved elasticity, wrinkle reduction, and wound healing acceleration. The investment is greater (reconstitution, injection, peptide cost) but the biological effect is stronger.
What does not work: expecting oral collagen supplements to match injectable peptide results, or expecting GHK-Cu to address systemic joint health the way oral collagen does. Each tool has its optimal use case. Use them together for complementary coverage.
