Why No One Talks About Peptide Drug Interactions
Search "peptide drug interactions" on any major drug interaction checker and you will get nothing useful. This is not because peptides do not interact with medications — they do. It is because the standard drug interaction databases (Lexicomp, Micromedex, Epocrates) catalog interactions between FDA-approved medications, and most peptides used in the optimization community are not FDA-approved.
The clinical reality: pharmacological interactions occur when one substance alters the absorption, distribution, metabolism, elimination, or pharmacological effects of another. Peptides have pharmacological effects — they activate receptors, modulate hormones, and alter physiological pathways. They interact with other substances that affect those same pathways. The absence of formal interaction databases does not mean the absence of interactions.
This guide covers the clinically significant interactions that are supported by pharmacological mechanism, clinical evidence, or established case reports. These are the interactions your physician may not warn you about because they are not in the standard databases — but they are real and they matter.
GLP-1 Agonists and Medication Timing
Semaglutide, tirzepatide, and retatrutide significantly delay gastric emptying — this is one of their primary mechanisms for appetite reduction. The clinical consequence: any orally administered medication may have altered absorption kinetics when co-administered with a GLP-1 agonist. Medications that are particularly affected:
(1) Oral contraceptives — delayed absorption may reduce peak levels and potentially decrease contraceptive efficacy. The FDA label for tirzepatide recommends switching to non-oral contraception or using barrier methods during dose escalation. (2) Levothyroxine — thyroid hormone replacement has narrow therapeutic windows. GLP-1-induced delayed absorption can cause variable thyroid levels. Monitor TSH more frequently during escalation. (3) Oral diabetes medications (metformin, sulfonylureas) — combined with GLP-1's insulin-potentiating effects, there is additive hypoglycemia risk. Sulfonylureas in particular should be dose-reduced when starting GLP-1 therapy. (4) Warfarin — delayed absorption leads to unpredictable INR levels. Monitor INR weekly during GLP-1 dose escalation.
The general rule: take critical oral medications at least 1 hour before GLP-1 injection, and be aware that absorption timing may shift during dose escalation when gastric motility effects are most variable.
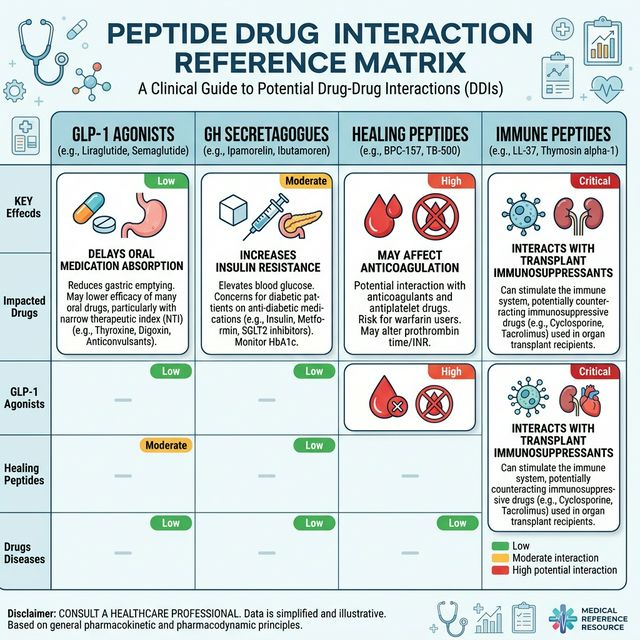
GH Secretagogues and Insulin Resistance
Growth hormone is a counter-regulatory hormone that opposes insulin action. All GH-elevating peptides (ipamorelin, CJC-1295, tesamorelin, hexarelin, MK-677, and exogenous GH) can increase insulin resistance and raise fasting blood glucose. The interactions that matter: (1) Insulin and insulin analogs — patients on insulin therapy may require dose adjustments when starting GH secretagogues. Monitor fasting glucose and HbA1c at baseline and every 4-6 weeks. MK-677 is particularly relevant here due to 24-hour sustained GH elevation.
(2) Metformin — this interaction is actually synergistic. Metformin improves insulin sensitivity and can counterbalance GH-induced insulin resistance. Some practitioners co-prescribe low-dose metformin (500-1000 mg/day) with GH secretagogues specifically for this purpose. (3) Sulfonylureas (glipizide, glyburide) — these drugs stimulate insulin secretion. The combination of sulfonylurea-induced insulin with GH-induced insulin resistance creates unpredictable glucose dynamics. Monitor closely.
(4) Corticosteroids (prednisone, dexamethasone) — both corticosteroids and GH increase blood glucose. The combination is additive and can cause clinically significant hyperglycemia. If you are on chronic corticosteroids, GH secretagogue use requires close glucose monitoring.
Healing Peptides and Blood Thinners
BPC-157 and TB-500 promote angiogenesis (new blood vessel formation) and wound healing, which involves coagulation cascade activation and platelet-mediated tissue repair. The interaction with anticoagulants is mechanistic: (1) Warfarin, heparin, enoxaparin — healing peptides may partially counteract anticoagulant effects at the local tissue level by promoting coagulation cascade components. This is a theoretical concern; no clinical studies have measured this interaction. However, patients on anticoagulation therapy should inform their prescriber about peptide use.
(2) Antiplatelet agents (aspirin, clopidogrel, prasugrel) — similar theoretical concern regarding healing peptide effects on platelet activation. More clinically relevant: if you are on antiplatelet therapy, subcutaneous injections may cause more bruising and prolonged bleeding at injection sites. Use smaller gauge needles (30-31g) and apply pressure for 60 seconds after injection.
(3) NSAIDs — BPC-157 may actually counteract NSAID-induced gastropathy, which is a beneficial interaction. However, NSAIDs' anti-inflammatory effects may partially counteract the inflammation-dependent healing pathways that BPC-157 and TB-500 utilize. Some practitioners recommend avoiding NSAIDs during active healing peptide protocols when possible.
Immunomodulatory Peptides and Immune-Active Medications
Thymosin Alpha-1, thymosin beta-4, and BPC-157 all have immunomodulatory properties. The interactions with immune-active medications are clinically important: (1) Immunosuppressants (cyclosporine, tacrolimus, mycophenolate, biologics) — thymosin alpha-1 stimulates T-cell function and enhances immune surveillance. In transplant patients on immunosuppression, TA1 could theoretically counteract the immunosuppressive effect and increase rejection risk. This is a serious contraindication that should be respected until data proves otherwise.
(2) TNF-inhibitors (adalimumab, infliximab, etanercept) — BPC-157 modulates TNF-α pathways. The interaction with exogenous TNF inhibition is undefined but theoretically could produce unpredictable immune modulation. Patients on biologics should discuss peptide use with their rheumatologist or immunologist.
(3) Immune checkpoint inhibitors (pembrolizumab, nivolumab) — these cancer drugs work by releasing immune system "brakes." Thymosin alpha-1's immune-stimulating effects could theoretically enhance checkpoint inhibitor efficacy but also increase immune-related adverse events. This interaction is being studied in oncology but is not yet defined for clinical guidance.
The overarching principle: if you are on any medication that modifies immune function, consult with the prescribing physician before adding any immunomodulatory peptide. The interactions are mechanistically plausible and the consequences of getting it wrong — especially in transplant, autoimmune, or oncology settings — are serious.