Two Fundamentally Different Philosophies
Testosterone Replacement Therapy (TRT) and peptide-based hormonal optimization represent opposing pharmacological approaches to the same clinical problem: declining testosterone levels.
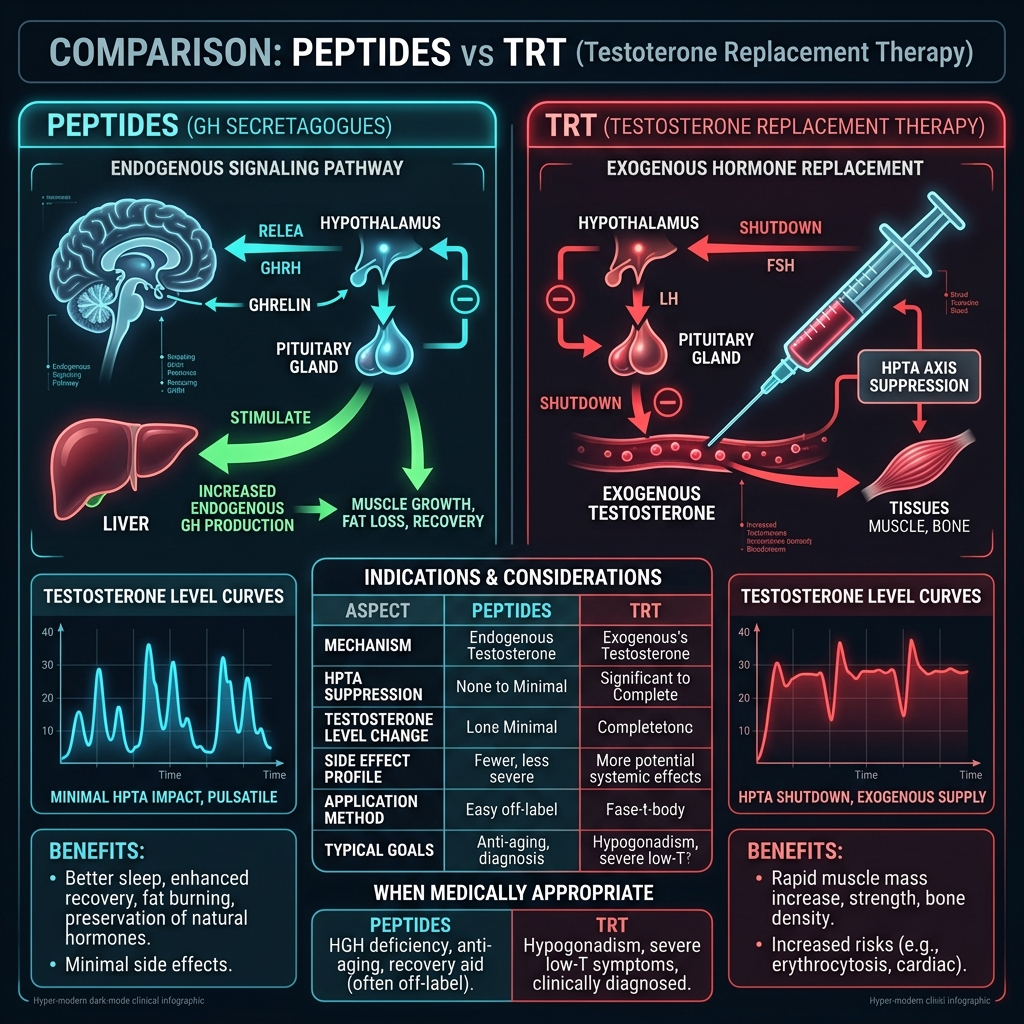
TRT (exogenous replacement): introduces synthetic testosterone directly into the bloodstream. The body detects supraphysiological testosterone and shuts down endogenous production via negative feedback at the hypothalamus and pituitary. The HPTA axis goes dormant. Result: guaranteed testosterone levels but complete dependency on continued administration.
Peptide optimization (endogenous stimulation): uses compounds like Kisspeptin-10, Enclomiphene, or GH secretagogues to stimulate the body's own hormonal production pathways. The HPTA axis remains active and functional. Result: more modest and variable testosterone elevation, but preserved biological autonomy.
TRT: Benefits and Tradeoffs
Benefits: rapid, predictable serum testosterone elevation to any target level (typically 800-1,200 ng/dL); elimination of symptoms (fatigue, low libido, cognitive fog) within 2-4 weeks; well-studied safety profile over decades of clinical use.
Tradeoffs: complete suppression of endogenous testosterone production; testicular atrophy (average 25-50% volume reduction within 6 months); suppressed spermatogenesis and potential infertility; estrogen management often required (aromatase inhibitors); hematocrit elevation requiring periodic blood donation; commitment to indefinite treatment — discontinuation causes severe hypogonadal symptoms.
Peptide Approach: Benefits and Tradeoffs
Benefits: preserved HPTA axis function; maintained testicular volume and spermatogenesis; natural pulsatile hormone release patterns; easier discontinuation without severe withdrawal; no hematocrit elevation concerns.
Tradeoffs: less predictable testosterone elevation (typically 30-60% increase from baseline); slower onset of benefits (4-8 weeks); requires more compounds and complexity (Kisspeptin + Enclomiphene + GH secretagogues); limited long-term safety data; higher cost per month than generic testosterone cypionate.
Peptide protocols cannot rescue a completely non-functional HPTA axis. If Leydig cells are severely damaged (primary hypogonadism), no amount of upstream signaling will restore testosterone production. A serum LH/FSH test distinguishes primary (high LH, low T) from secondary (low LH, low T) hypogonadism.
Decision Framework
Choose TRT if: diagnosed primary hypogonadism, not planning future children, want maximum predictability, willing to commit to lifelong treatment.
Choose peptides if: secondary hypogonadism (functional HPTA axis), fertility preservation is important, prefer maintaining endogenous production, want the ability to discontinue without severe consequences.
Hybrid approach: some clinicians prescribe low-dose TRT (100-120 mg/week) combined with HCG (500 IU 2x/week) to maintain testicular function, then add Kisspeptin or Enclomiphene during planned "off" periods to accelerate HPTA recovery.